Acumen Suite: Market Access Tools
Policy Reporter’s suite of Market Access Tools are powered by our patented real-time payer intelligence software, providing you with the latest coverage data. Whether your drug is on the medical or pharmacy benefit, Policy Reporter captures live criteria, restrictions, preferred status and more in our interactive and easy-to-use dashboards.
Our Coverage Viewer tool is a powerful, user-friendly search interface to learn about your drugs coverage criteria across almost all Payers in the U.S.
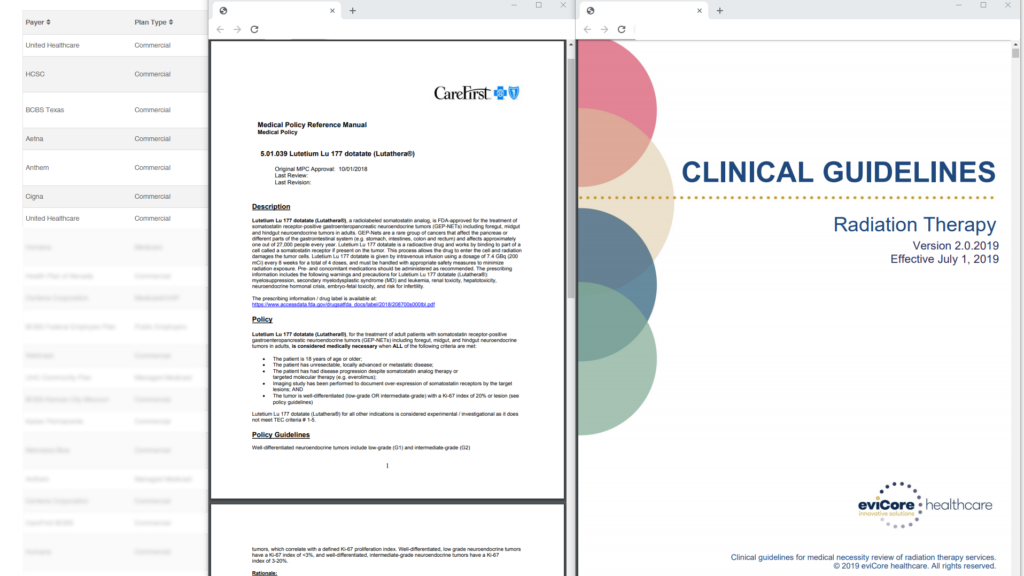
Utilizing Policy Reporter’s proprietary Payer policy tracking software, Coverage Viewer provides in-depth breakdowns of how Payers are covering your drug, in what states, and under what plan types. An invaluable tool for keeping abreast of the ever-changing Payer policy landscape.
The Coverage Viewer is a great tool to support your Sales & Market Access teams quickly analyze coverage of your drug, and inform providers of coverage plans.
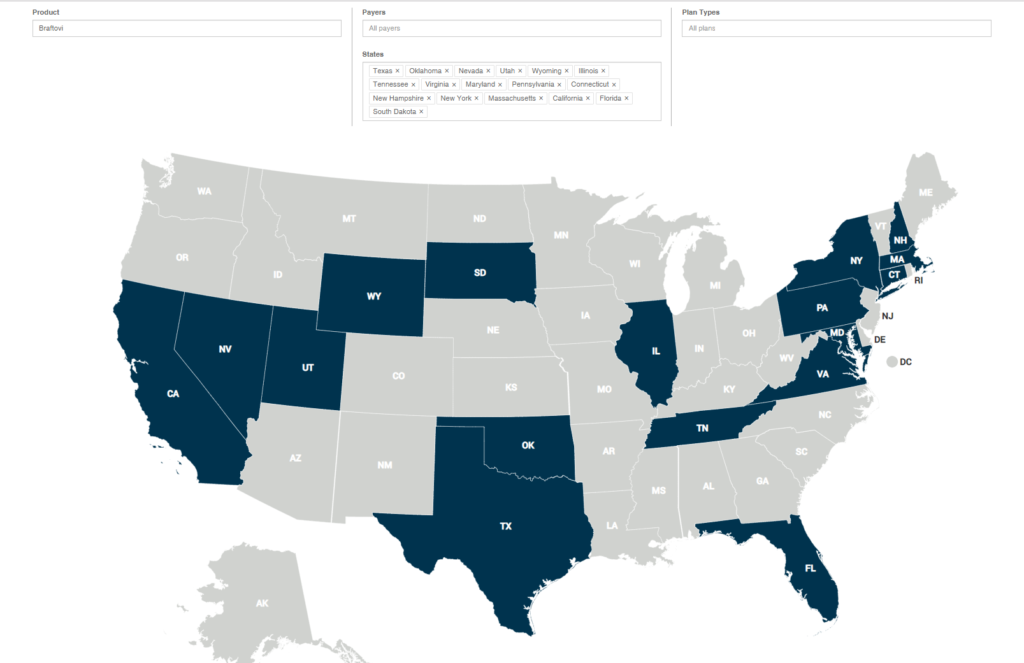
Informing Your Providers
Our tool enables your team to export either a simplified or detailed summary of coverage criteria for easy access to providers offline.
At each provider meeting, your account manager can bring this summarized report, which highlights coverage for your therapeutic by plan.
Ask our sales team for a demo today.
Book a demoPolicy Reporter’s Formulary Viewer provides real-time formulary reporting and analytics through a unique, patent-pending technology that ensures you're constantly accessing a live state of the market.
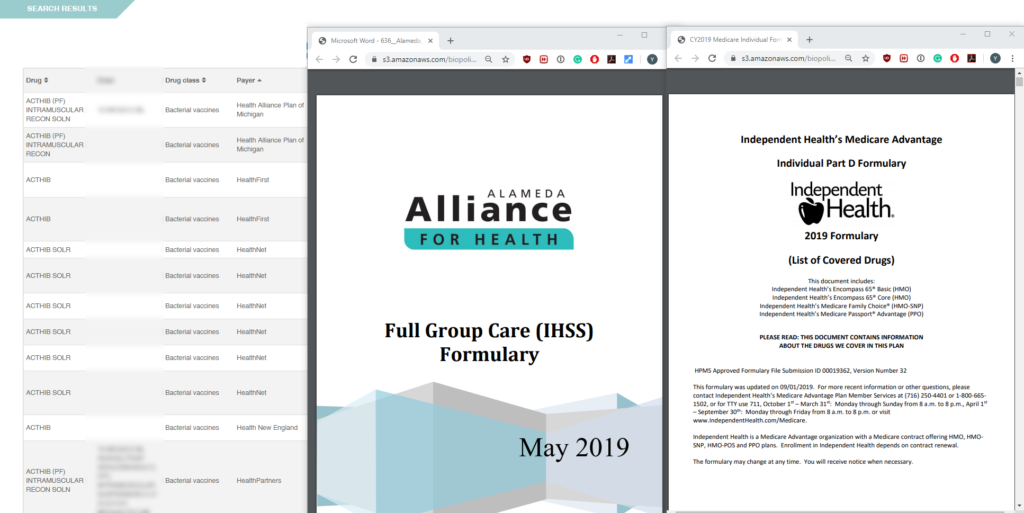
Understand and Track Tier Placement and Formulary Restrictions
Our Formulary Viewer allows users to search through various formulary criteria to find how your product is treated in the market. Users gain a unique, immediate insight into the breadth and restrictiveness of their drug coverage through granular search filters. Our dashboard gives users unprecedented search capabilities by offering a vast amount of search filters, including
- Drug class(es)
- Drug indication(s)
- Drug name(s)
- Payer Groups (e.g. Commercial Plans, Pharmacy Benefit Manager, Radiology Benefit Manager, etc.)
- Payers
- and More!
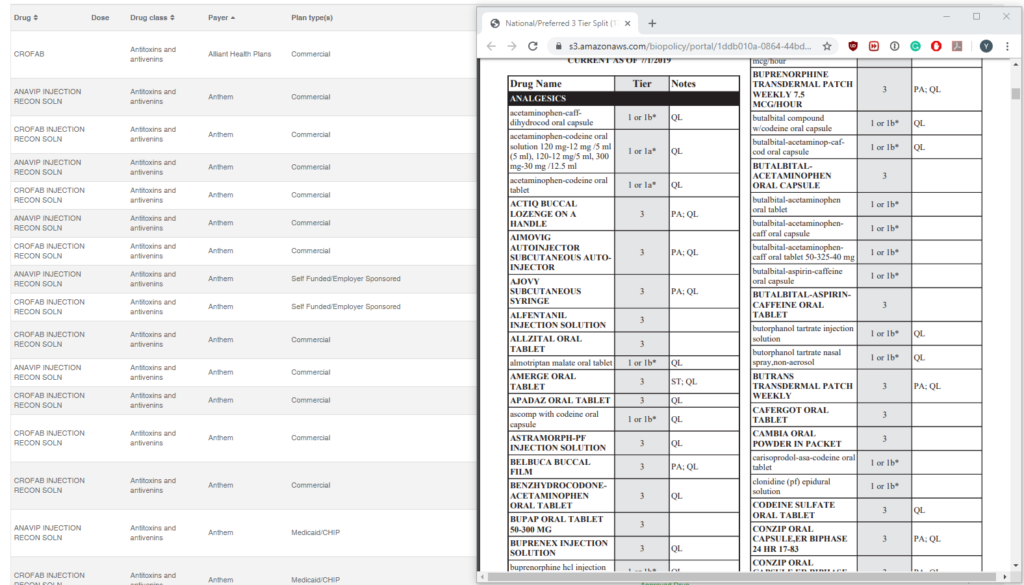
Empower your sales and market access teams to become an authority on how your drug is treated in the marketplace, ask our sales team for a live demo today.
Book a Demo
